Imagine running a hospital where every piece of equipment ventilators, MRI scanners, or patient beds is exactly where it’s needed, no matter the situation. Whether it’s a quiet day or a sudden flu outbreak, having the right tools at the right time can save lives and keep operations smooth.
Care Program Management (CPM) makes this possible by using smart, scenario-based planning to match equipment to patient needs. In 2025, 72% of healthcare facilities are adopting predictive tools like CPM to manage resources effectively.
The Goal: Equipment Ready for Patients
Hospitals strive to deliver top-notch care without delays, and that starts with having the right equipment in the right place. CPM takes this goal further by planning for different scenarios, like seasonal illnesses or unexpected emergencies. It ensures that resources, from life-saving ventilators to diagnostic tools, are available where and when patients need them most.
The vision is a healthcare system that’s always prepared, efficient, and focused on delivering the best care possible. By anticipating needs, CPM helps hospitals avoid the chaos of shortages or wasteful overstock, creating a system that supports both patients and staff.
The Problems: Why Equipment Planning Is Tough
Managing medical equipment is no easy task. Patient demand can change quickly one day a hospital might need extra beds for a surge in admissions, and the next it might face a shortage of diagnostic machines.
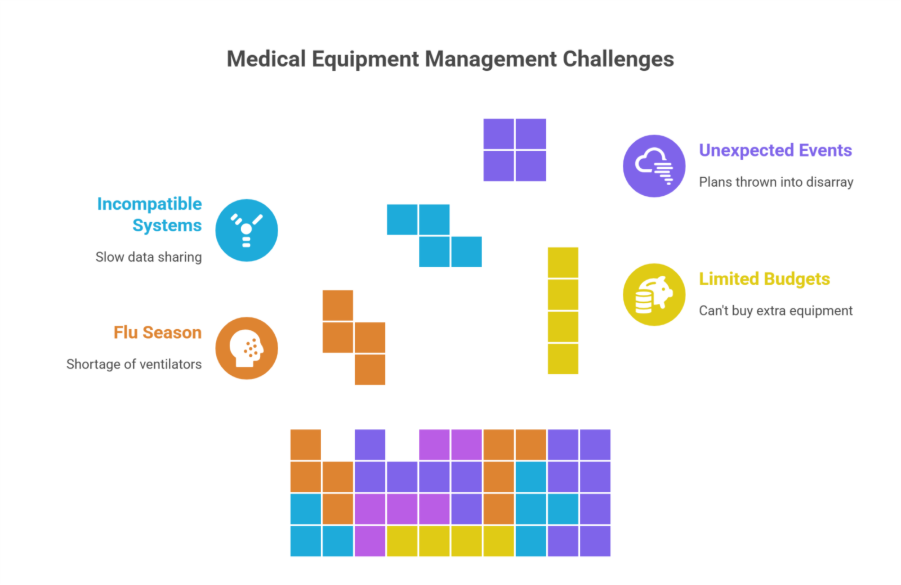
For example, during a flu season, a hospital might find itself short on ventilators, causing delays in critical care. Budgets are another hurdle where hospitals often can’t afford to buy extra equipment “just in case.” Sharing data between facilities, especially in a large network, is often slow and messy due to incompatible systems.
And unexpected events, like a sudden outbreak or natural disaster, can throw even the best plans into disarray. In 2026, these challenges can lead to misallocated resources, putting patient care at risk and driving up costs.
How CPM Helps: A Real-World Example
CPM uses scenario-based planning to prepare for equipment needs before shortages occur. A mid-sized hospital network learned this firsthand after its urban facility ran out of ventilators during a severe flu outbreak last winter.
With CPM, the network analyzed past flu data and local health trends, which pointed to a 20% rise in ventilator demand for winter 2025. At the same time, the rural hospital showed surplus capacity. The system recommended moving 10 ventilators to the city ahead of time while keeping five in reserve.
The plan worked because CPM connected the dots drawing from patient records, usage logs, and even weather patterns while coordinating transfers and checking maintenance standards. When flu season arrived, the urban hospital had the equipment it needed. And when a small COVID-19 cluster appeared, CPM quickly redirected diagnostic tools to the affected site, ensuring care wasn’t disrupted.
CPM focuses on several key areas:
-
Program coordination: Aligns equipment across departments and facilities.
-
Demand prediction: Uses data to forecast needs for specific scenarios, like flu season or emergencies.
-
Resource alignment: Matches tools to where they’re needed most, like ventilators in high-demand areas.
-
Data insights: Pulls together information from multiple sources to guide decisions.
-
Adaptability: Adjusts plans when unexpected events occur.
-
Cost efficiency: Stretches budgets by avoiding unnecessary purchases.
-
Readiness: Keeps hospitals prepared for any situation.
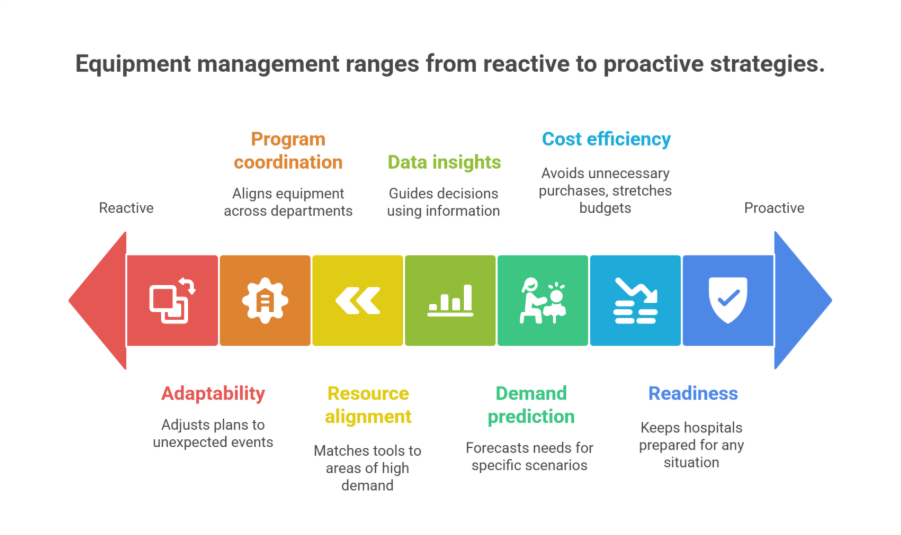
With data volumes in healthcare rising nearly 50% annually, CPM’s predictive framework is set to become even more powerful turning real-time insights into early interventions
~Bloomberg
Why It Matters: Real Benefits for Hospitals
CPM delivers practical benefits that directly impact hospitals and patients. In the hospital network example, coordinated planning prevented ventilator shortages during a flu surge, ensuring timely care and avoiding last-minute scrambles for equipment.
By predicting demand, CPM kept rural hospitals from holding unused ventilators while urban ones faced shortages. Data-driven insights, like analyzing past flu trends, gave managers confidence to act early. Flexibility also proved critical, allowing the network to respond quickly when a COVID-19 cluster appeared. And by reallocating existing equipment instead of buying new, the network saved thousands of dollars.
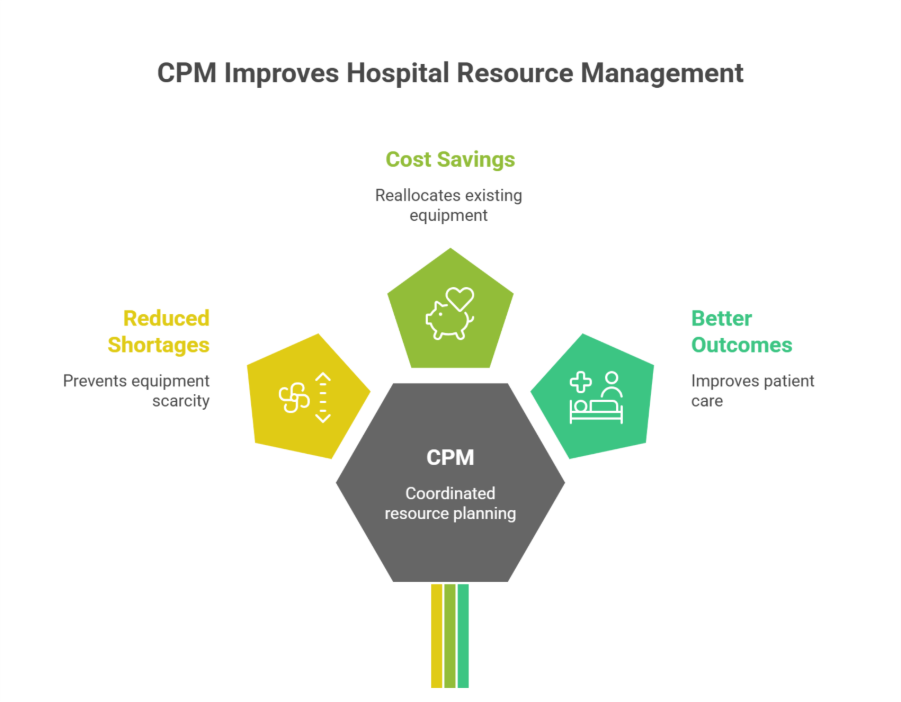
These advantages extend beyond one case. CPM streamlines equipment use across entire networks, reducing waste and ensuring critical tools are available where they’re needed most. It helps managers anticipate shortages, reallocate resources during busy periods, and handle unexpected events such as outbreaks or equipment failures.
The result is better patient outcomes, improved staff efficiency, and meaningful cost savings that can be reinvested in areas like training or facility upgrades. With more than 70% of healthcare facilities adopting predictive tools, CPM is already proving its value in strengthening both care quality and financial health.
What’s Next: The Future of CPM
By 2025, CPM could redefine hospital resource planning. No longer limited to flu season prep, advanced systems may spot unusual surges from pediatric spikes to specialized surgical demands by pairing AI with real-time data from patient records, supply chains, and even global health alerts.
That kind of foresight could warn hospitals of a looming ventilator shortage weeks before it happens. But hurdles remain: staff must be trained to act on predictions, IT systems upgraded for live data sharing, and strict privacy rules observed. Budgets, too, will weigh heavily, forcing hospitals to balance upfront costs against future savings.
Still, the promise is clear: hospitals that embrace CPM could emerge more efficient, resilient, and prepared for whatever comes next.






